TLDR/Summary
- I recently presented our new research on Covid-19 outcomes (watch the recording embedded above – 37min, moderately technical), revisiting what analysts got wrong about pandemic preparedness and why.
- Pandemics remain a major global risk, and emerging AIxBio threats make it critical we understand what actually drives good pandemic outcomes.
- Early Covid-19 analyses were misleading due to flawed data (especially underreporting of deaths) and poor statistical methods.
- Our new, more robust analyses show that pandemic preparedness, measured by the Global Health Security (GHS) Index, does predict lower excess mortality, especially in non-island countries.
- Islands had fundamentally different pandemic experiences, with lower mortality driven by geography and border control strategies, so they must be analysed separately.
- Key structural factors differ by context: democracy mattered more in islands, while low inequality was more important for non-islands, highlighting that preparedness interacts with broader social conditions.
- The video above explains the technical details of all of this.
- You can download the slides here.
- Many thanks to my collaborators on this Covid-19 work: Nick Wilson, Michael G Baker, & Amanda Kvalsvig
Pandemics are still a major global threat
Pandemics remain one of the most significant global catastrophic risks. Covid-19 demonstrated not only the scale of harm that infectious disease can cause, but also how deeply uncertain our understanding of pandemic performance can be.
Looking forward, emerging risks at the intersection of artificial intelligence and biotechnology (AIxBio) could further amplify these threats. It is critical that the world correctly understands what determines good pandemic outcomes.
Much analysis on pandemic preparedness is flawed
A key debate during Covid-19 was whether traditional measures of pandemic preparedness actually mattered. Early in the pandemic, many analyses suggested that they did not.
The Global Health Security (GHS) Index, which purported to assess countries’ pandemic preparedness, appeared to have little or no explanatory power for Covid-19 outcomes. Some studies even found that higher-scoring countries performed worse.
These findings fed into a broader narrative: that “soft” factors such as trust, social cohesion, and low corruption mattered more than formal preparedness; that authoritarian regimes may have had an advantage; and that wealthier countries fared worse than expected.
However, these conclusions were based on early pandemic data and that data turned out to be deeply flawed.
As demonstrated in the presentation above, Covid-19 mortality reporting varied systematically across countries. Countries with stronger institutions, often those with higher GHS Index scores, were better at detecting and reporting deaths. Conversely, some countries with apparently “good” outcomes were simply undercounting mortality. When analyses relied on reported cases or deaths, they risked measuring data quality rather than pandemic performance. Similar confounding occurred due to the different age-structures of populations.
In addition, early studies often failed to account for key statistical issues. Variables such as GDP and mortality were highly skewed, yet were frequently analysed without transformation. As illustrated in the presentation above, applying appropriate transformations can substantially change results, sometimes eliminating spurious relationships altogether.
The key lesson is this: when analyses produce results that fly in the face of our a priori evidence-based hypotheses and expectations, we shouldn’t accept results uncritically. We must ask, why did the expected result not appear, what might be wrong with the data or our analysis?
Pandemic preparedness saves lives
More recent work, including our own research on the Covid-19 pandemic, using improved data and methods, tells a very different story. In the video above, I explain the technical details of why this occurred.
When excess mortality is used (rather than reported deaths), when age structure is accounted for, and when appropriate statistical transformations are applied, the GHS Index does in fact predict pandemic outcomes. For example, analyses such as that of Ledesma et al. (2023) showed a clear negative relationship between preparedness and mortality once some of these corrections are made.
In our own work, which carefully addressed additional critiques of the Ledesma et al. study, we find similar patterns: higher GHS scores are associated with lower excess mortality, particularly in non-island countries.
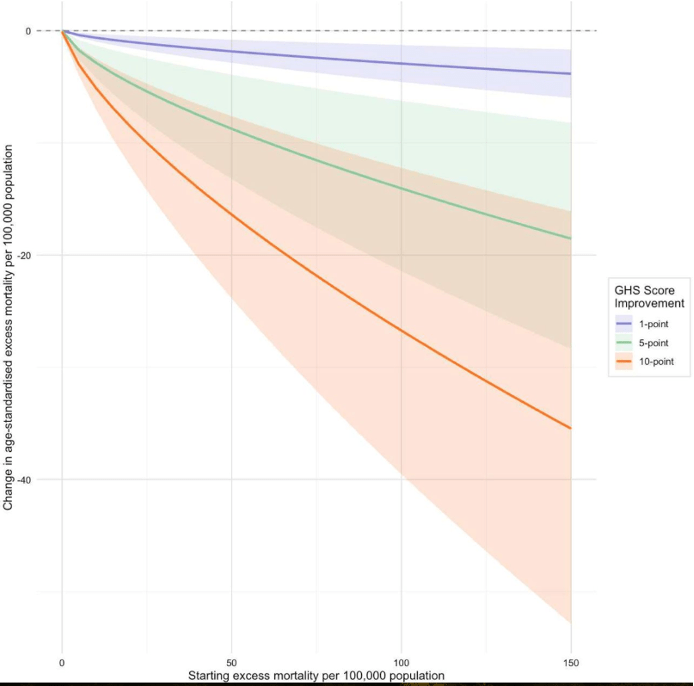
This reversal highlights a critical lesson: data quality and analytical choices matter enormously. Early pandemic narratives, while understandable given the urgency of the moment, were often based on incomplete or misleading evidence (as explained in the presentation above).
As better data has become available, some widely repeated claims now need to be reconsidered or reversed. Unfortunately some of the slogans emerging from these early analyses, and widely shared, have now established themselves as dis-informative slogans.
Islands experienced the pandemic very differently
Another key insight from our analysis is that not all countries should be treated as a single group. Islands, in particular, had a fundamentally different pandemic experience.
Historically, islands have had distinct advantages in infectious disease control, and Covid-19 was no exception. Island jurisdictions experienced dramatically lower excess mortality on average than non-islands. This reflects both geography and strategy: islands can more effectively implement border controls, and many pursued elimination strategies that were simply not available, or not chosen, elsewhere.
Because of these differences, combining islands and non-islands in a single analysis can obscure important relationships. When we separate them, clearer patterns emerge.
In non-island countries, preparedness, as captured by the GHS Index, strongly predicts outcomes. In islands, however, geography and border strategy play a much larger role, and preparedness metrics may behave differently. Many islands succeeded during Covid-19 despite their poor pandemic preparedness. But this pattern does not generalise to the non-island jurisdictions of the world.
Enhancing democracy and reducing inequality matter
The impact of structural factors also vary between these groups. Our results suggest that, among islands, democratic governance is associated with better outcomes, likely reflecting the importance of public consent and compliance in border-based strategies and elimination of local outbreaks.
In contrast, among non-islands, lower inequality appears to be a key determinant, perhaps because more equitable societies are better able to sustain collective action and protect vulnerable populations.
These findings help reconcile some of the apparent contradictions in early pandemic analyses. It is not that preparedness “doesn’t matter”, but rather that its effects interact with geography, strategy, and social structure in complex ways. The impact of preparedness, democracy’s crisis advantage, and inequality, are conditional on the context, and mutually reinforcing.
Islands should leverage their advantages
Finally, there may be broader lessons from island epidemiology. Islands have long been sites of successful infectious disease control, including the elimination of zoonotic diseases such as hydatid disease and brucellosis in some settings, and strong biosecurity responses to threats like avian influenza, which remains absent from New Zealand, Australia, and many Pacific Islands as at the time of writing. Their geographic isolation can enable tighter control over animal and human movement, reducing opportunities for pathogen introduction and spread.
This raises an intriguing possibility: that the advantages islands demonstrate in pandemic control may generalise to other infectious disease risks, particularly those involving zoonotic spillover. If so, understanding how island systems manage biosecurity could offer valuable insights for strengthening global preparedness, especially in an era of increasing biological risk.
As we prepare for future pandemics, the lesson is clear. Preparedness does matter, but only if we measure it properly, analyse it carefully, and understand the contexts in which it operates.
